Authors: Lucia Saborido and Gisela Garcia-Alvarez, CSG Cluster Saúde de Galicia

As IN-4-AHA is coming to an end we want to emphasize the bigger picture and analyze the connections between tools and outputs of Working Packages (WPs) Innovation Scaling Model (WP3), Test and Validation Activities to Design Scalable Solutions (WP4) and Impact Assessment and Governance Data (WP5) as well as the digital tools developed along this project.
We could say that WP3 is the backbone ensuring long-term cooperation within the healthcare ecosystem by building a connected knowledge base that considers existing solutions and provides a validated model for the co-design process of innovation in the healthcare and social care sectors. A participatory design review and participation in workshops have been carried out that offered a set of tools to engage the end users of the innovative solutions and allow an exchange of views among all stakeholders.
This network of stakeholders involved in the health and social context, are the ones that have been selected to carry out the testing and validation activities to design scalable WP4 Solutions Accessibility mapping and adoption of services and products, where end users are elderly people and their formal and/or informal caregivers. In addition, service providers have used the tools shown in participatory design workshops such as the Decide method, priority mapping, and impact effort mapping to decide the scope of testing. To define the profile of the elderly people who participate in the tests according to each of the projects selected in the open call for living labs, goal-setting workshops have been used. For the testing phase in the living labs, tools such as the Understand method, the Assumption Collecting method, Service Map and Five Why’s have been used to collect feedback from end users. Other tools used in WP4 task 4.2 have been focus groups to map end-user accessibility where families, professionals, seniors and members of the IN-4-AHA consortium have participated.
The business coaching portion of the living lab tests from WP4, T4.1Living Lab Scaling Up and Innovation Manual, has used several participatory design tools such as the Evaluate method, the Ideas method, the Framing method and the Storyboards method.
For WP5 Impact assessment and governance data, a wide range of participatory methods have been used to gather information from stakeholders. In addition, a survey of the service providers selected in the open call has been carried out to explore their use of impact assessment and a map of data management practices. WP5 and WP3 Innovation Scaling Model held a joint participatory workshop to present the initial structure of the Data Management Guide.
Success for a public-private collaboration, analyzed under task 3.2, is based on mutual understanding of goals and how to achieve them, having a joint agreement on success indicators at the end of the project, and having clear expectations about what will happen if there is success. In addition, strong institutional support helps the dialogue between the public and private sectors to have a better collaboration. This collaboration is also reviewed in WP6, T6.3 Investment strategy implementation, where one of the activities is to promote the culture of cross-border impact investing through public and private procurement of innovation.
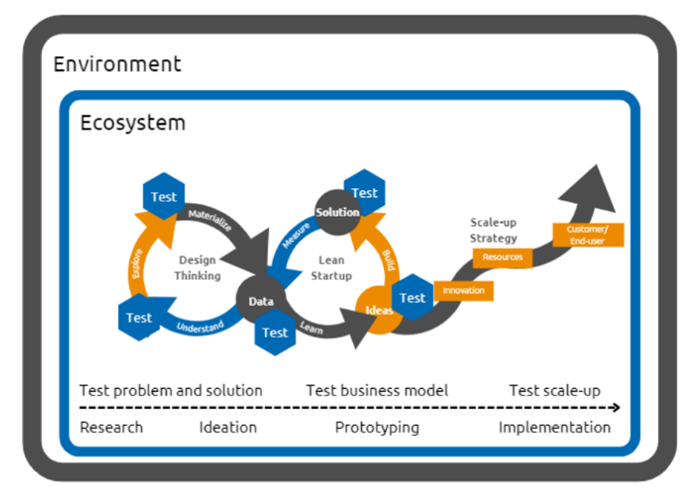
In summary, the factors that help innovation succeed is that the unmet challenge or need is demand-driven and the solution must be developed jointly between the demand side and the supply side as co-creation. In addition, innovation must adapt easily to daily routines, be easy to use and be reliable. This relates to the T4.1 playbook in Chapter 2 which explains what scaling innovation is and the importance of understanding the customer’s problem. Also in the conclusions of the playbook one of the principles that could help startups is to involve all relevant stakeholders where the recipients of AHA solutions are not only elderly end users, but also those in their environment. This includes family members, national, regional, and local governments, care providers, and other service
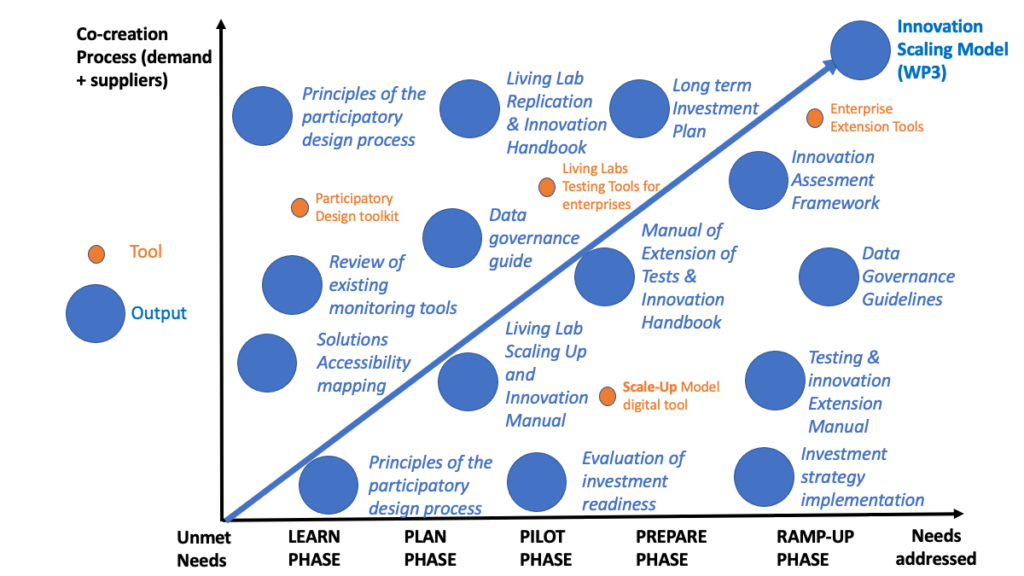
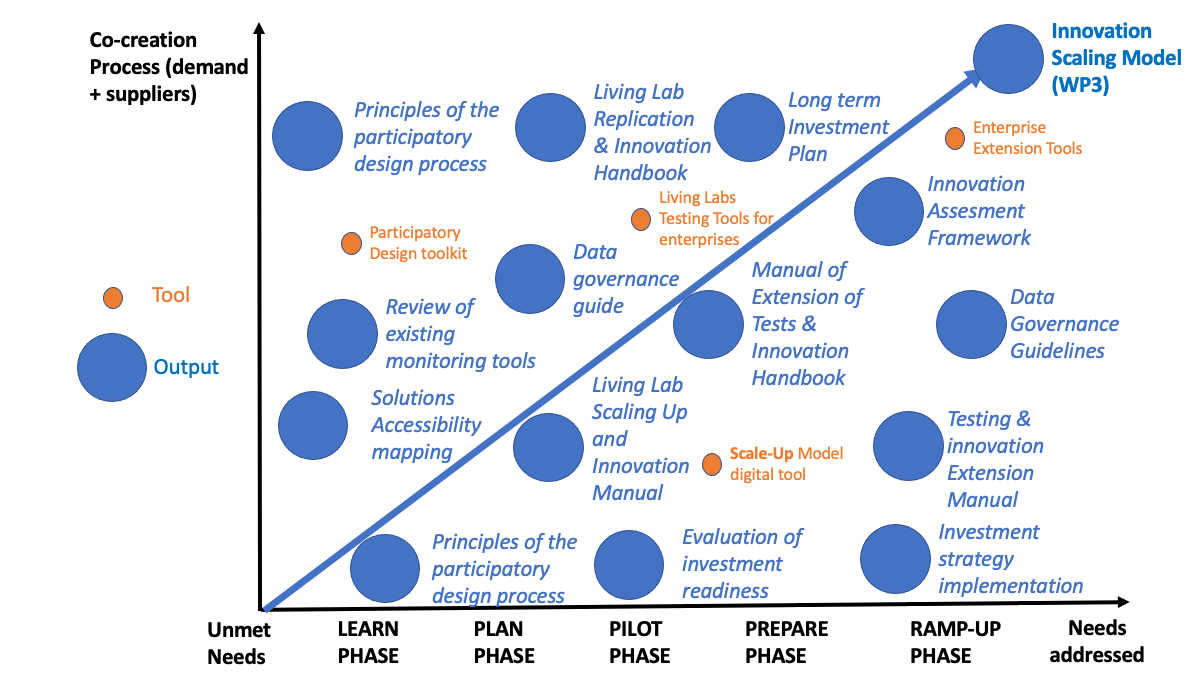
The Innovation Scale-Up Model and Roadmap consists of five phases, starting with general information gathering (LEARN) and followed by concentrated efforts to prepare for a pilot project (PLAN). After testing the solution in the target market (PILOT), it is necessary to evaluate all the information collected and establish a detailed plan to implement scaling (PREPARE). Only when proper preparations are made is it reasonable for the solution owner to enter the large-scale target market (RAMP-UP).
In the LEARN phase, the deliverable 3.1 Principles of the participatory design process through participatory design methods and tools has been taken into account. In addition, the participation of all stakeholders and the identification of end users of the deliverable is also relevant. 4.2 Mapping accessibility and adoption of services and products and the deliverable 4.1 Living Lab Testing and Innovation Scale-Up Manual, Questionnaires addressed to service providers have also been taken into account, service users and facilitators due to the importance of the person-centered approach to contribute to the successful adoption of the solution found in the deliverable 5.1 Review of existing monitoring tools. For the financial part, the information in 6.1 Evaluation of the preparation of the investment has been taken into account.
In the PLAN phase, a review of the legal and regulatory environment of the markets is made, so the data governance guide of deliverable 5.3 has been taken into account. In addition, the innovation evaluation questionnaire for end-users has also been taken into account. Se refers to the main factor contributing to successful adoption which is the person-centered approach present in the deliverable 4.2 Mapping accessibility and adoption of services and products and the deliverable 4.1 Living Lab Replication and Innovation Handbook.
In the PILOT phase, a small-scale adoption of the solution is carried out and the learnings and protocols of the deliverable 4.2 Accessibility mapping and adoption of services and products and the tool that measures the focus present in innovative solutions together withthe deliverable 4.1 Manual of extension of tests and innovation of Living Lab is taken into account.
In the PREPARE phase the company of the innovative solution must establish a tactical plan to initiate and execute a large-scale implementation in the target market. Reference is made to the information in Living Lab’s Deliverable 4.1 Testing and Innovation Extension Manual.
In the RAMP-UP phase, innovation has entered the target market and all components already evaluated in the previous phases must continue to be monitored and evaluated. Reference is made to Living Lab’s 4.1 Testing and Innovation Extension Manual.
At a cross-cutting level and common to all phases, information on the guidelines of the innovation assessment framework of deliverable 5.2 has been used. Reference is also made in all phases to the investment resources present in the deliverable 6.2 Long-Term Investment Plan.
The development of the roadmap for the implementation of the innovation scaling model has been made a reference document for all stakeholders involved in scaling up innovative solutions in the field of health and care that is also relevant for the preparation of policies, investment strategies, communication and promotional activities. For the overall description of the process, goals and expected outcomes and indicators relevant to the success of the scaling process, the AHA’s 5.2 Innovation Assessment Framework and the 5.3 Data Governance Guidelines deliverable have been taken into account. For recommendations on public-private partnership, reference is made to deliverable 3.2 Recommendations on public-private partnership. Content of the deliverable 6.1 Evaluation of the disposition of the investment and the content of the playbook of the deliverable 4.1 have also been taken into account. In addition, an analysis of accessibility and adoption of the solutions and a review of the content of the focus groups has been carried out, referring to the deliverable 4.2 Mapping of accessibility and adoption of services and products and the deliverable 3.1 Participatory design.
The Scale-Up Model digital tool has been developed from the 3.3 Innovation Scale-Up Model and Roadmap, which is intended for companies whose innovative solution already has feasibility testing at local, regional or national scale, but whose ambition is to expand into new international markets. The model also serves as a tool for industry support organizations: clusters, accelerators and others, so that they can help their members throughout the enlargement process.
Digital tools developed at IN-4-AHA
The participatory design process toolkit is a support tool to create value in small and medium-sized enterprises to evaluate their innovative solution. It is also an interesting tool for policymakers and health authorities as it helps to understand why innovative solutions need to be implemented.
And also this tool helps investors to better understand the potential of the innovative solution and to participate in the development of the solution from an early stage.
This tool has been made thanks to the contents of the deliverables 6.2 Long-term investment plan, which explains the development path for digital health solutions classified as medical devices, the deliverable 4.1 Living lab testing and innovation playbook (chapter 2), the deliverable 3.1 Principles of the participatory design process and the needs of the large-scale innovation process in the health and care sector, the deliverable 4.2 Accessibility mapping and adoption of services and products and the deliverable 5.3 Data governance guidelines.
The living labs testing tools for enterprises are in the digital version of deliverable 4.1 within the playbook.
- The Living Lab Test Preparation tool allows innovators to define their goals, needs and expectations for living lab testing and has been conducted through a series of interviews with living lab coordinators in the IN-4-AHA project.
- The Living Lab Test Preparation: Solution, Prerequisites and Testing Needs tool serves to acquire information about the pilot solutions and has been conducted through a series of interviews with living lab coordinators in the IN-4-AHA project.
- The Estimating the values of person-centred care tool helps estimate the values of person-centred care that should be taken into account for the adoption of innovation. This tool collects the opinions of the participants in the focus groups carried out within the deliverable 4.2 Mapping accessibility and adoption of services and products.
- The Technology Readiness Assessment (TRL) tool serves to describe each TRL (Technology Readiness Levels) and provides checklists to determine if the technology is in that specific TRL.
Enterprise extension tools are also found in the digital version of deliverable 4.1 within the playbook.
- The tool Key points of a business model (Lean Canvas) serves to think about the answers and the collection of them.
- The Evaluation of the scalability of an innovation tool is used to evaluate the scalability of the innovation.
- The tool Improving the scalability of an innovation serves to identify actions that can contribute to improving scalability.
- The Questions to Consider tool when expanded. Why, what and how? It serves to identify what questions need to be answered when developing a strategy to scale up innovation.